Урология №2 (supplement) / 2017
Мочекаменная болезнь
Мочекаменная болезнь (МКБ), несмотря на значительные достижения как в диагностике, так и в лечении, продолжает занимать важное место в повседневной практике уролога и практикующих врачей общего профиля.
В основе развития МКБ лежат нарушения обменных процессов, связанных как с алиментарными факторами, так и с заболеваниями эндокринной системы, наследственной предрасположенностью, а также c климатогеографическими условиями.
В среднем риск заболеваемости уролитиазом колеблется от 1 до 20% [1]. Заболеваемость уролитиазом среди мужчин выше, чем среди женщин (соотношение около 3:1), и наиболее часто проявляется в возрасте 35–50 лет, однако в последние десятилетия это соотношение имеет обратную тенденцию: так, по данным Stamatelou и соавт., на основании регистра NHANES эта пропорция составила 1,75 к 1 [2].
Распространенность МКБ зависит от географических, климатических, этнических, диетических и генетических факторов. Риск рецидива определяется, преимущественно, заболеванием или нарушением, которое привело к образованию камня. Показатели распространенности МКБ варьируют от 1% до 20%. Встречаемость достаточно высокая в странах с высоким уровнем жизни, например в Швеции, Канаде или США (>10%). В некоторых регионах отмечается увеличение заболеваемости более чем на 37% за последние 20 лет.
Камни можно классифицировать по причинам их образования: инфекционные, неинфекционные, вследствие генетических дефектов или образовавшиеся при приеме лекарственных препаратов (лекарственные) (табл. 1).
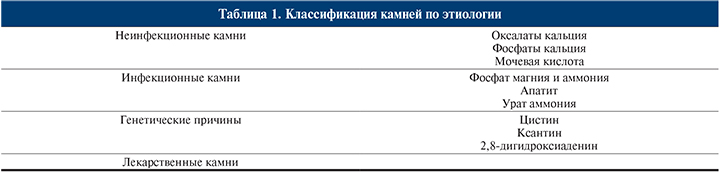

Минералогический состав камней
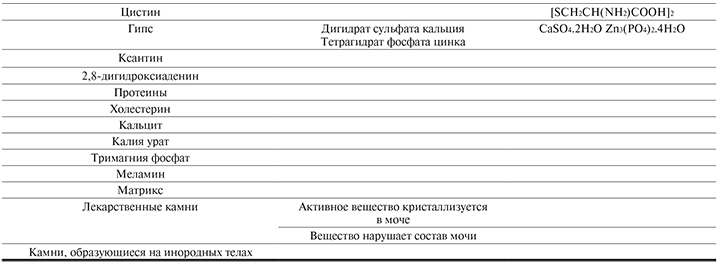
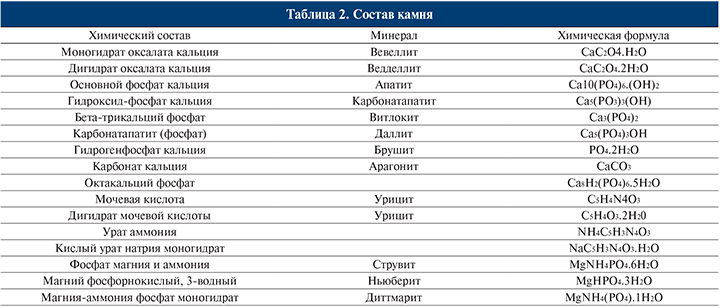
Состав камня служит основой для диагностики и определения тактики лечения. Клинически наиболее значимые минеральные составляющие мочевых камней перечислены в табл. 2.

Факторы и группы риска камнеобразования
 Учитывая высокий риск рецидивирования, а именно порядка 50% пациентов с МКБ имеют минимум 1 рецидив, от 10 до 20% – 3 рецидива и более [3, 4], знание факторов риска имеет наиважнейшее значение (табл. 3).
Учитывая высокий риск рецидивирования, а именно порядка 50% пациентов с МКБ имеют минимум 1 рецидив, от 10 до 20% – 3 рецидива и более [3, 4], знание факторов риска имеет наиважнейшее значение (табл. 3).
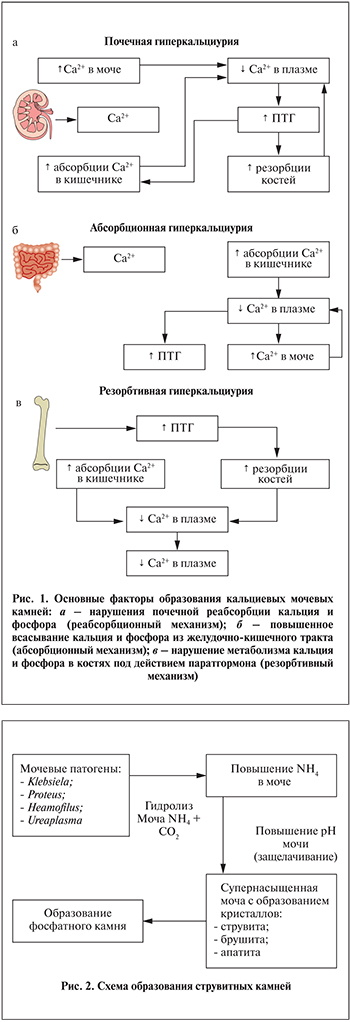
Среди факторов, влияющих на формирование кальциево-оксалатных камней, часто можно выявить заболевания эндокринной системы (паращитовидных желез), желудочно-кишечного тракта и непосредственно почек (тубулопатии). Нарушение пуринового обмена приводит к уратному нефролитиазу. К развитию гиперкальциемии, гиперфосфатемии, гиперкальциурии и гиперфосфатурии приводят заболевания, представленные на рис. 1.
Хронические воспалительные заболевания мочеполовой системы могут способствовать образованию инфицированных фосфатных (струвитных) камней (рис. 2).
В зависимости от факторов и развивающихся метаболических нарушений формируются различные по химическому составу мочевые камни.
Классификация химических видов камнеобразующих веществ
- Неорганические камни:
- при рН мочи 6,0 – кальций-оксалат (вевелит, веделит);
- при рН мочи 6,5 – кальций-фосфат (гидроксил-карбонатапатит);
- при рН мочи 7,0 – магний-аммоний-фосфат (струвит).
 Кальциевые камни (обнаруживают у 75–85% больных) чаще находят у мужчин старше 20 лет. Рецидив регистрируют в 30–40% наблюдений (брушит – в 65%).
Кальциевые камни (обнаруживают у 75–85% больных) чаще находят у мужчин старше 20 лет. Рецидив регистрируют в 30–40% наблюдений (брушит – в 65%).
Струвитные камни связаны с инфекционным агентом. Их выявляют в 45–65% случаев, чаще у женщин. Отличаются высоким риском воспалительных осложнений. Рецидив заболевания быстрый (до 70%) при неполном удалении камня и отсутствии лечения.
- Органические камни:
- при рН мочи 5,5–6,0 – мочевая кислота, ее соли (ураты), цистин, ксантин;
- при рН мочи 6,0 – уратаммония.
Цистиновые (1%) и ксантиновые камни связаны с врожденными нарушениями обмена веществ на уровне организма в целом. Рецидив достигает 80–90%. Метафилактика крайне сложна и не всегда эффективна.
Таким образом, под сочетанным воздействием экзогенных, эндогенных и генетических факторов происходят нарушения метаболизма в организме, сопровождаемые усилением выделения почками камнеобразующих веществ.
Процесс формирования камня может быть длительным и нередко протекает без клинических проявлений, что наиболее характерно для коралловидных камней, а может проявиться острой почечной коликой, обусловленной отхождением микрокристалла.
К сожалению, действующая в настоящее время классификация МКБ не отражает всех клинических форм мочекаменной болезни и не позволяет дать правильную оценку активности процесса, эффективности лечения и адекватно интерпретировать осложнения.
Теории камнеобразования
Существует несколько теорий камнеобразования, каждая из которых имеет право на существование:
- Матричная теория, в основе которой лежат инфекция и десквамация эпителия, закладывающие ядро формирующегося камня.
- Коллоидная теория – когда защитные коллоиды переходят из лиофильного состояния в лиофобное, создавая благоприятные условия для патологической кристаллизации.
- Ионная теория базируется на недостато...












